HOME / ARTICLES / COVID-19 AND LIGHT PROGRESS
COVID-19: Our UVGI Solutions
03.19.2020
At this time of global crisis due to the effects of the spread of Covid-19, Light Progress is receiving a significant number of requests from all over the world. Our systems safeguard people’s health and enable healthcare professionals to work much more safely.
UV – C EFFICACY AGAINST CORONAVIRUSES (SARS – MERS)
Our company has always been committed to preventing contamination and increasing safety by controlling cross-contamination in all areas: surface treatment, air quality, and water purification. UVGI is an established and reliable technology, but solid know-how is required for effective and safe use. UVGI uses ultraviolet light to inactivate microorganisms by cross-linking thymidine nucleotides in DNA and uracil nucleotides in RNA, which block replication. UVGI systems are relatively fast and easy to use, leave no chemical residues, and do not expose workers to harmful substances. Currently, there are no specific tests on UV resistance of Coronavirus SARS-Cov-2. Still, there are examples of scientific literature about the UV-C treatment of very similar viruses, such as SARS or MERS.
There is also evidence of the effectiveness of ultraviolet rays in disinfecting air and surfaces from microorganisms that are much more complex and difficult to treat than this virus. These include C. Difficile, MRSA, or even more deadly threats such as Ebola and Legionella. (Kowalski 2009) It is estimated that the SARS-CoV-2 virus can survive on surfaces for up to nine days, based on its similarity to SARS and MERS.
Standard disinfectants are effective against SARS-CoV-2, but to provide additional protection and defend against errors in the manual disinfection process, UVGI can be used to disinfect surfaces and equipment following manual chemical disinfection. “ASHRAE” (American Society of Heating, Refrigerating and Air-Conditioning Engineers) recommends ultraviolet germicidal irradiation to address disease transmission of COVID-19.
UV irradiation in air conditioning and air treatment systems has been recommended for many years. Light Progress UV systems for air conditioning are already widely used in many sectors: hospitals, industry, transport networks, and residential centers. For more information, see the HVAC section of our website.
SANITIZE MASKS WITH UVGI
UVGI has been successfully tested in laboratories to decontaminate N95 masks exposed to MS2 bacteriophage and influenza virus.
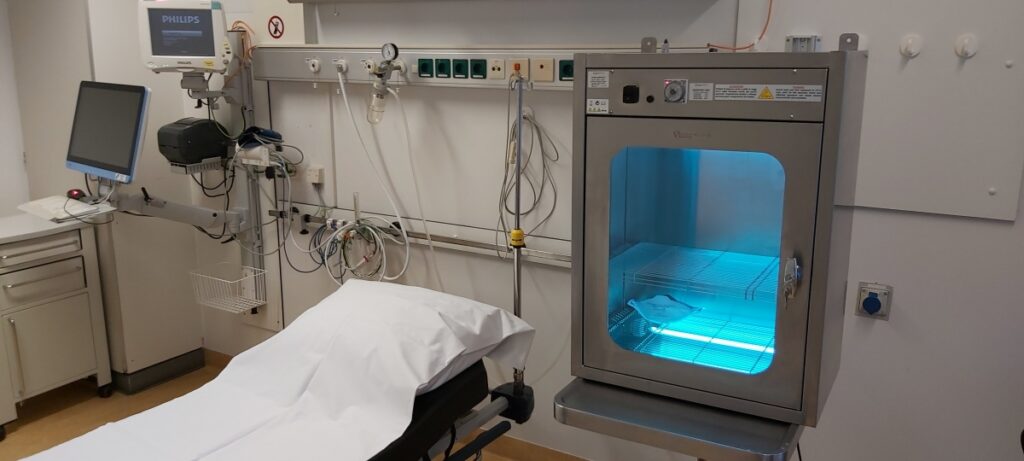
In recent weeks our distribution network in the healthcare sector has been working non-stop. Our partners are professionals and experts in infection control, and they have provided us with numerous application ideas, which can – or indeed, must – be shared as much as possible. Lights4Health, our partner in the Netherlands, has just provided the SEH department (First Aid) at Leiden University Medical Center with UV treatment cabinets. The systems will disinfect N65 masks in use by medical and paramedical staff.
Two studies on the UV-C treatment of masks were published in leading scientific journals in 2015 and 2018, respectively, well before the recent release of Covid-19.
-
National Institutes of Health: Effects of Ultraviolet Germicidal Irradiation (UVGI) on N95 Respirator Filtration Performance and Structural Integrity
-
American Journal of Infection Control: Ultraviolet germicidal irradiation of influenza-contaminated N95 filtering facepiece respirators
The problem of finding masks is a constant in analyzing possible “apocalyptic” scenarios regarding managing a global pandemic. One of the texts reports:
“The possibility of a global pandemic of an infectious respiratory disease is of tremendous concern to the occupational health community because healthcare workers would face the most significant risk of exposure. For pandemic diseases that airborne particles may transmit, the isolation precaution guidelines from the Centers for Disease Control and Prevention (CDC) call for healthcare workers to wear respiratory protection while treating patients. Because of their loose fit and low filtration capacity, surgical masks do not provide respiratory protection against tiny airborne particles.
For this reason, the most common respiratory protection device in healthcare settings is the disposable N95 filtering facepiece respirator (FFR). However, infection control procedures typically require disposable FFRs to be discarded after a single use to avoid cross-contamination. This means that a pandemic of a disease such as influenza would require a tremendous number of FFRs to protect healthcare workers from airborne transmission. The Institute of Medicine (IOM) projected that a 6-week influenza pandemic would require 90 million FFRs. The Occupational Safety and Health Administration (OSHA) has predicted that an influenza pandemic would likely last 24 weeks, which suggests that up to 360 million FFRs could be needed in the United States alone. A surge in demand of this magnitude would significantly exceed current stockpiles and production capabilities and almost certainly result in a shortage.”
During the 2009 H1N1 pandemic, the CDC (“Centers for Disease Control and Prevention” USA) recommended that healthcare facilities consider extending the use and reuse of N95 respirators in cases of extreme need. One way to meet the growing demand for masks during a pandemic would be to reuse them. This is because even a small number of reuses of each mask would greatly expand the available stock of disposable respirators. Buying masks in bulk represents a high cost, in addition to the difficulties associated with the production and distribution processes.
However, a significant concern for reuse is the possibility that the external surfaces of the respirator may become contaminated with infectious material and lead to disease transmission. To avoid this risk, masks should be decontaminated after each use. Several techniques have been tested for the decontamination of N95 FFR. These include autoclaves, steam generated by heat or microwaves, ethylene oxide, vaporized hydrogen peroxide, and bleach. All the methods described have advantages and disadvantages. Heat and moisture, for example, may dissolve or degrade the respirator and require the device to dry after treatment. Chemical disinfectants require rinsing and drying and may leave an unpleasant odor or residue that irritates the skin. Gaseous systems using ethylene oxide or vaporized hydrogen peroxide require specialized equipment and ventilation controls.
MASKS DECONTAMINATION WITH UVGI: RISKS AND OPPORTUNITIES
N95 systems cannot be disinfected with alcohols such as isopropanol because they remove the electrostatic charge from the filtration medium and substantially degrade its filtration capacity. An imperative consideration for all decontamination methods, including UVGI, is the risk that they degrade the respirator material. This will reduce the ability of the mask to filter out infectious bioaerosols.
Some studies have examined the effects of UVGI on the respirator’s appearance, fit, airflow resistance, and filtration efficiency after one or three decontamination cycles and found no significant impact. However, the effects of prolonged UVGI exposure after multiple decontamination cycles are unknown. How much can a cumulative dose of UVGI respirators withstand, what damage will occur at the end, or how many times can disposable masks be decontaminated and reused?
This suggests that the upper limit for UVGI exposure during repeated disinfection cycles should be set by physical degradation of the respirator material. This should be determined by the loss of filtration capacity. For some FFR models, this could be a helpful warning: if the respirator material is significantly degraded after UVGI disinfection, the mask should be discarded.
For even more effective action, it is advisable to subject the mask to dry heating at around 60°C. This will inactivate potential infectious nuclei trapped within the filter weave as much as possible. Of course, it would be desirable to have sufficient time and possibilities to quickly design N95 masks specifically for healthcare professionals that can be disinfected even 50 times with UV-C disinfection cycles in less than 60 seconds. However, the current situation makes this operation impractical.
UV-BOX AND MORE: LIGHT PROGRESS SOLUTIONS TO SANITIZE MASKS AND TOOLS IN HEALTHCARE
Based on feedback from our sales network, UV-BOX has proven effective in treating masks and all material contained in an ambulance during the current Covid-19 emergency.
Due to the need to transport patients and the short time between calls, Leiden University Medical Center decided to treat potentially contaminated material with our UV system. An indicator that changes color when sufficient UV radiation is achieved to inactivate the surface pathogens was used to confirm the correctness of the treatment.
Besides masks, our UV-BOX can be used to treat any other tool, such as instruments commonly used in hospitals, clinics, ambulances, etc. Light Progress also designed a specific device for stethoscope decontamination using innovative UV-C LED, a medical device class I, CE registered with the Ministry of Health, FDA approved. Healthcare environments have always been protected from possible contamination with Light Progress products. Everybody should be aware that at this time of absolute global crisis, UVGI technology can make a difference in how we control contamination spread, safeguarding patients’ and workers’ health.
UVGI technology creates no resistance in microorganisms to ensure constant efficacy and excellent effectiveness, proven by science. Many applications are possible, not only in healthcare environments. Visit our website for more information. The COVID-19 emergency requires the commitment of everyone. Light Progress is willing to provide its products at discounted prices to meet the market’s growing demands and contribute during this time of extreme difficulties.
Bibliography:
Lindsley WG, Martin SB Jr, Thewlis RE, et al. Effects of Ultraviolet Germicidal Irradiation (UVGI) on N95 Respirator Filtration Performance and Structural Integrity. J Occup Environ Hyg. 2015;12(8):509–517. doi:10.1080/15459624.2015.1018518 Ultraviolet germicidal irradiation of influenza-contaminated N95 filtering facepiece respirators” Mills, Devin et al. American Journal of Infection Control, Volume 46, Issue 7, e49 – e55 Kowalski, Wladyslaw. (2020). 2020 COVID-19 Coronavirus Ultraviolet Susceptibility. 10.13140/RG.2.2.22803.22566. Hang L, Yang Y-R, Zhang Z, Lin Z. (2020). Genomic variations of COVID-19 suggest multiple outbreak sources of transmission. medRIX (preprint). 20. Zhu N, Zhang D, Wang W, Li X, Yang B, Song J, Zhao X, Huang B, Shi W, Lu R and others. (2020). “A Novel Coronavirus from Patients with Pneumonia in China”, 2019. N Engl J Med 382,727-733. Hang L, Yang Y-R, Zhang Z, Lin Z. (2020). “Genomic variations of COVID-19 suggest multiple outbreak sources of transmission.” medRIX (preprint).
Light Progress takes no responsibility for mask degradation using our UVGI systems; all products must be used consciously.
